Embryo Quality Problems in IVF
A Complete Guide to Understanding Why Embryos Fail to Implant
Embryo quality is one of the most important factors determining whether an IVF cycle results in pregnancy. Even when fertilization occurs successfully and embryos appear normal under ... Even when fertilization occurs successfully and embryos appear normal under the microscope, hidden genetic or biological problems may prevent implantation or cause early miscarriage. Understanding embryo quality problems is essential for couples who have experienced failed IVF cycles, repeated implantation failure, or embryos that stop growing in the laboratory.

What Does “Embryo Quality” Actually Mean?
Embryo quality refers to how healthy and capable an embryo is of developing into a successful pregnancy. During IVF, eggs are fertilized with sperm in a laboratory and begin dividing into multiple cells. Over several days, these cells continue dividing and forming an early-stage embryo. Embryologists carefully monitor this development and evaluate embryos based on how normally they grow.
However, appearance alone does not tell the full story. An embryo may look perfectly healthy under a microscope but still carry genetic abnormalities that prevent implantation. This is why embryo quality involves multiple biological factors including:
Key Factors Affecting Embryo Quality
- Chromosomal integrity
- Egg quality
- Sperm DNA quality
- Cell division patterns
- Metabolic health of embryo cells
- Genetic stability during development
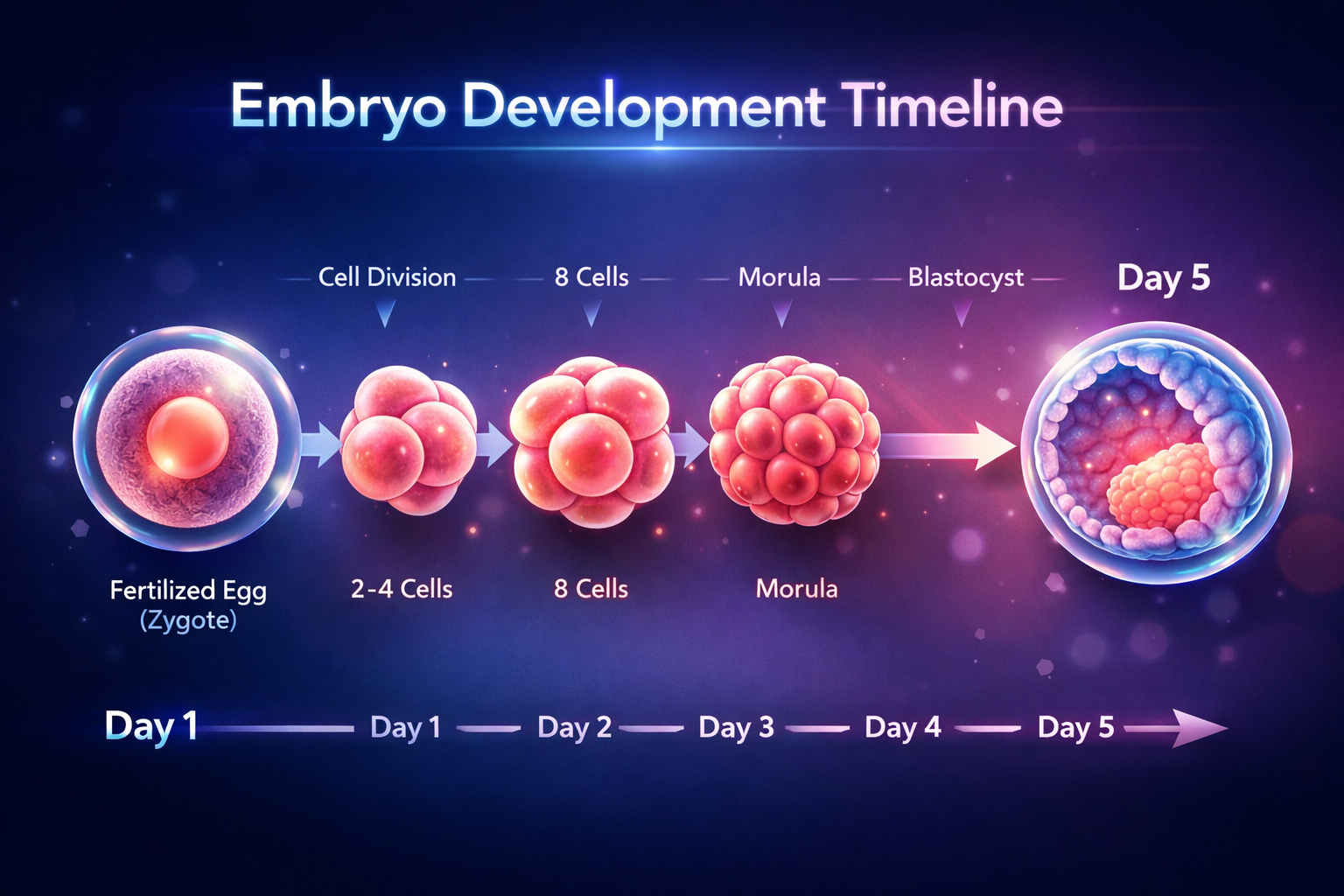
Normal embryo development timeline from fertilization (Day 1) to blastocyst stage (Day 5).
How Embryos Normally Develop During IVF
Understanding the stages of embryo development helps explain why some embryos stop growing before reaching the blastocyst stage.
Embryos that successfully reach the blastocyst stage generally have a higher implantation potential. When embryo development stops before day 5, it may indicate genetic abnormalities, poor egg or sperm quality, or laboratory factors.
Day 1
Fertilization occurs when the sperm successfully penetrates the egg, forming a single cell called a zygote.
Day 2
The embryo begins dividing into multiple cells and typically reaches the 2–4 cell stage.
Day 3
The embryo continues dividing and usually reaches the 6–8 cell stage. Doctors assess cell symmetry and fragmentation.
Day 4
Cells compact together forming a structure known as a morula as the embryo prepares for blastocyst formation.
Day 5
The embryo becomes a blastocyst with an inner cell mass and outer trophoblast layer, ready for implantation.
Common Embryo Quality Problems
Chromosomal Abnormalities (Aneuploidy)
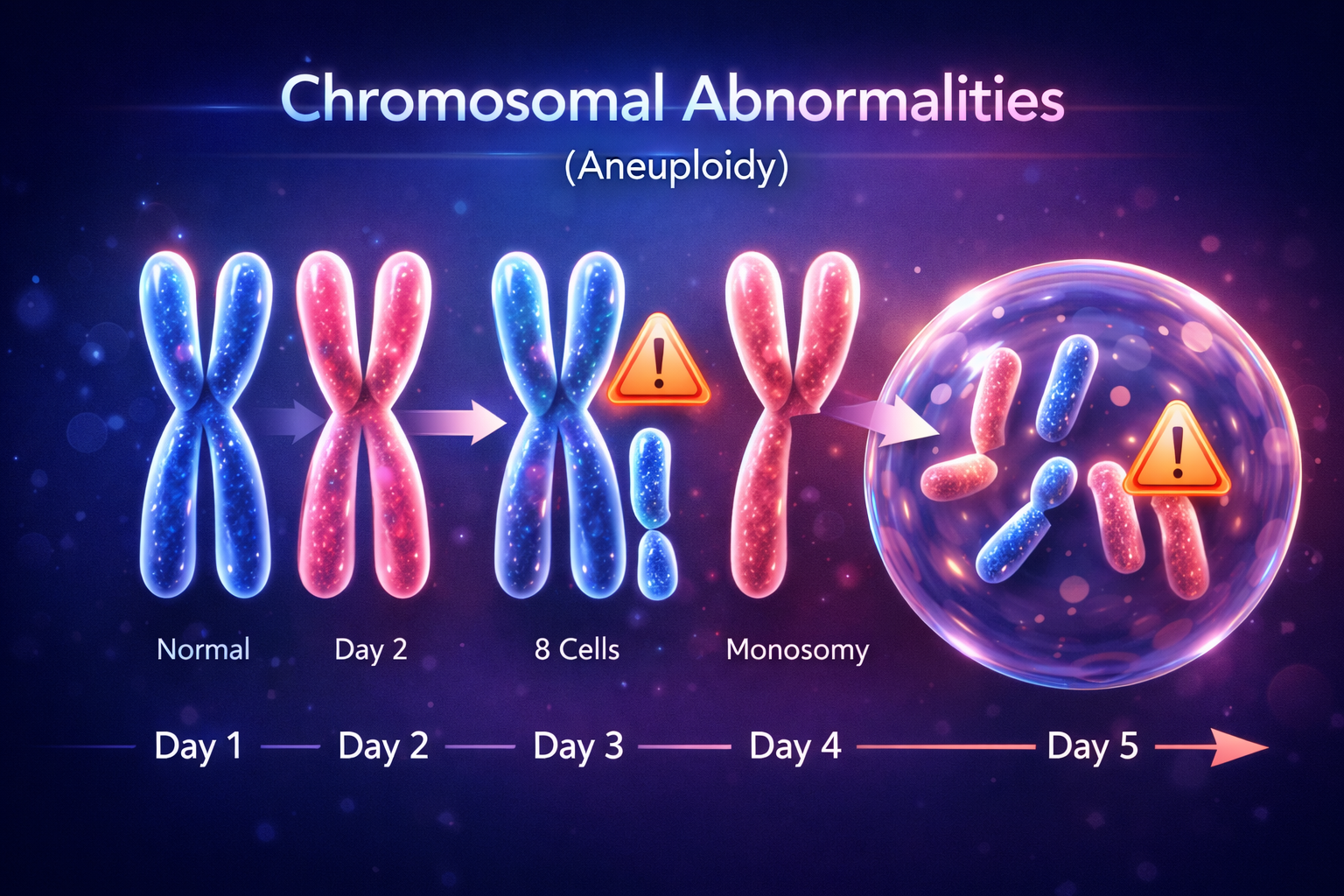
Illustration showing how extra or missing chromosomes (aneuploidy) affect embryo development.
One of the most common reasons embryos fail to implant is chromosomal abnormalities. Humans normally have 46 chromosomes. If an embryo has extra or missing chromosomes, normal development becomes difficult or impossible. These abnormalities often occur due to errors during egg cell division and become more common with increasing maternal age. Embryos with severe chromosomal abnormalities may fail to implant, stop developing, or lead to miscarriage.

Comparison between a healthy egg and poor-quality egg affecting embryo development in IVF.
Poor Egg Quality
Egg quality declines naturally with age, especially after age 35. Poor egg quality can lead to abnormal embryo development, chromosomal errors, and reduced implantation potential. Eggs also contain mitochondria that provide energy for early embryo development. When mitochondrial function declines, embryo growth may be affected.
Embryo Fragmentation

Illustration showing how embryo fragmentation affects embryo quality during IVF development.
Fragmentation refers to small fragments of cellular material that appear between embryo cells during development. A small amount of fragmentation is common, but high levels may interfere with normal cell division and reduce the embryo’s ability to develop properly. more>>

Illustration showing embryos that arrest before reaching the blastocyst stage in IVF development.
Embryos That Stop Growing Before Day 5
Some embryos begin dividing normally but suddenly stop growing after a few days. This developmental arrest may occur due to chromosomal abnormalities, poor egg quality, sperm DNA damage, or metabolic problems within the embryo. more>>
Genetic Mutations Affecting Development

Illustration showing how inherited genetic mutations may affect early embryo development.
Some embryos inherit genetic mutations from parents that affect early development. These mutations may interfere with cell signaling, organ development, or chromosome stability. In certain cases, preimplantation genetic testing (PGT) may help identify embryos without specific genetic conditions.
Confused about your IVF embryo report?

Doctors evaluate embryo quality using microscopy, embryo grading, genetic testing, and advanced monitoring systems.
How Doctors Evaluate Embryo Quality
- Embryo grading by experienced embryologists
- Blastocyst development assessment
- Preimplantation Genetic Testing (PGT-A)
- Sperm DNA fragmentation testing
- Evaluation of ovarian reserve
- Egg quality assessment
Strategies That May Improve Embryo Quality

Multiple clinical and lifestyle strategies may help improve embryo quality and IVF success rates.
- Optimizing ovarian stimulation protocols
- Improving egg and sperm health before IVF
- Using advanced embryo culture technology
- Genetic testing to select healthy embryos
- Addressing hormonal or metabolic issues
- Improving lifestyle factors such as diet, sleep, and stress
- Personalized IVF treatment planning
Embryo Grading Explained
Embryologists use embryo grading to evaluate the appearance and development of embryos during IVF. While grading does not guarantee pregnancy success, it helps doctors identify embryos that appear most capable of implantation.
Day-3 Embryo Grading
At the cleavage stage (Day-3), embryos usually contain between six and eight cells. Embryologists assess several factors including the number of cells, symmetry of cells, and the amount of fragmentation present.
| Grade | Description |
|---|---|
| Grade A | Even cells with minimal fragmentation |
| Grade B | Minor irregularities in cell size |
| Grade C | Noticeable fragmentation |
| Grade D | Poor cell structure |

Day-5 blastocyst grading evaluates expansion stage, inner cell mass, and trophectoderm quality.
Day-5 Blastocyst Grading
Blastocyst grading is more detailed and evaluates three components:
- Blastocyst expansion stage
- Inner cell mass (future fetus)
- Trophectoderm cells (future placenta)
Blastocysts are typically graded using a combination such as AA, AB, BB, or BC. AA embryos are considered excellent quality, while lower grades may have reduced implantation potential but can still result in healthy pregnancies.
Day-3 vs Day-5 Embryo Transfer

Comparison between Day-3 embryo transfer (cleavage stage) and Day-5 blastocyst transfer in IVF treatment.
One of the most common decisions in IVF treatment is whether embryos should be transferred on Day-3 or Day-5. Both approaches have advantages and are chosen based on patient history and embryo development.
Day-3 Transfer
Day-3 transfer involves placing embryos into the uterus when they are still in the cleavage stage. This approach is often used when the number of embryos is limited or when embryos struggle to survive in laboratory culture. Advantages of Day-3 transfer include earlier placement in the natural uterine environment and reduced risk of embryos stopping development in the lab.
Day-5 Transfer
Day-5 transfer uses blastocyst embryos that have developed further. Because embryos must survive several days of development, blastocysts are often considered more viable. Blastocyst transfer also allows doctors to select embryos with the highest developmental potential, which may increase implantation rates.
Real IVF Cases With Embryo Quality Issues
Case 1: Repeated IVF Failure Due to Chromosomal Abnormalities
A 38-year-old patient underwent three IVF cycles with good fertilization rates but repeated implantation failure. Genetic testing later revealed that most embryos carried chromosomal abnormalities, explaining the failed transfers.
Case 2: Poor Embryo Development Due to Sperm DNA Damage
Another couple experienced embryos that consistently stopped growing before Day-5. Further testing showed high sperm DNA fragmentation levels. After treatment and lifestyle changes, embryo development improved in the next cycle.
Case 3: Laboratory Conditions Affecting Embryo Growth
In some situations, embryo culture conditions may impact development. Advanced culture systems and time-lapse monitoring have improved embryo survival in modern IVF laboratories.
Are Embryo Quality Problems Affecting Your IVF?
If your IVF cycle produced poor-quality embryos or embryos that stopped growing, a detailed case review may help identify the underlying cause and guide your next treatment.
उम्मीद अभी बाकी है
Expert IVF Review
Personalized insights based on your reports
Common Embryo Quality Myths
Myth 1: Poor-Grade Embryos Never Lead to Pregnancy
Many patients believe that only top-graded embryos can result in pregnancy. In reality, lower-grade embryos can still implant and lead to healthy babies.
Myth 2: Embryo Quality Depends Only on the Woman
Sperm quality plays a major role in embryo development. DNA damage in sperm can contribute to poor embryo development or developmental arrest.
Myth 3: IVF Laboratories Always Produce Perfect Embryos
Even in the best laboratories, some embryos naturally fail to develop due to genetic issues beyond medical control.
Why Some Embryos Stop Growing Before Day-5
One of the most frustrating situations during IVF treatment occurs when embryos begin developing normally but suddenly stop growing before reaching the blastocyst stage. This phenomenon is known as embryo developmental arrest. It usually happens between Day-3 and Day-5 of embryo development. For many couples, the fertilization report initially looks promising. Eggs fertilize successfully, and embryos divide normally during the first few days. However, when the laboratory checks the embryos later, development has stopped and the embryos never reach the blastocyst stage.
Understanding why embryos stop developing is important because it often reveals deeper biological issues affecting fertility.
Chromosomal Abnormalities
The most common cause of embryo arrest is chromosomal abnormalities. A normal human embryo should contain 46 chromosomes — 23 from the egg and 23 from the sperm. If an embryo has missing or extra chromosomes, its development can become unstable. Many abnormal embryos begin dividing normally during the first few days but cannot continue development beyond the cleavage stage. As a result, they stop growing before reaching the blastocyst stage.
Egg Quality Problems
Egg quality plays a crucial role in early embryo development. Eggs provide the cellular machinery and energy required for cell division during the first several days after fertilization. When egg quality declines — which commonly happens with increasing maternal age — embryos may struggle to divide properly or may stop growing during development.
Sperm DNA Damage
Although sperm contributes only half the genetic material, sperm DNA quality can significantly influence embryo development. High levels of sperm DNA fragmentation can interfere with normal embryo growth and lead to developmental arrest. In some couples with repeated IVF failures, specialized testing such as sperm DNA fragmentation testing may reveal underlying male factor issues affecting embryo quality.
Embryo Metabolic Problems
Embryos require energy to continue dividing and developing. This energy comes from mitochondria within the egg cells. If mitochondrial function is impaired, embryos may lack sufficient energy to complete development.
Laboratory Conditions
Although modern IVF laboratories are highly controlled environments, embryo culture conditions can still influence development. Temperature fluctuations, culture media quality, and oxygen levels can all impact embryo growth.
Why Some Embryos Stop Growing Before Day-5
One of the most frustrating situations during IVF treatment occurs when embryos begin developing normally but suddenly stop growing before reaching the blastocyst stage. This phenomenon is known as embryo developmental arrest. It usually happens between Day-3 and Day-5 of embryo development. For many couples, the fertilization report initially looks promising. Eggs fertilize successfully, and embryos divide normally during the first few days. However, when the laboratory checks the embryos later, development has stopped and the embryos never reach the blastocyst stage.
Understanding why embryos stop developing is important because it often reveals deeper biological issues affecting fertility.
Chromosomal Abnormalities
The most common cause of embryo arrest is chromosomal abnormalities. A normal human embryo should contain 46 chromosomes — 23 from the egg and 23 from the sperm. If an embryo has missing or extra chromosomes, its development can become unstable. Many abnormal embryos begin dividing normally during the first few days but cannot continue development beyond the cleavage stage. As a result, they stop growing before reaching the blastocyst stage.
Egg Quality Problems
Egg quality plays a crucial role in early embryo development. Eggs provide the cellular machinery and energy required for cell division during the first several days after fertilization. When egg quality declines — which commonly happens with increasing maternal age — embryos may struggle to divide properly or may stop growing during development.
Sperm DNA Damage
Although sperm contributes only half the genetic material, sperm DNA quality can significantly influence embryo development. High levels of sperm DNA fragmentation can interfere with normal embryo growth and lead to developmental arrest. In some couples with repeated IVF failures, specialized testing such as sperm DNA fragmentation testing may reveal underlying male factor issues affecting embryo quality.
Embryo Metabolic Problems
Embryos require energy to continue dividing and developing. This energy comes from mitochondria within the egg cells. If mitochondrial function is impaired, embryos may lack sufficient energy to complete development.
Laboratory Conditions
Although modern IVF laboratories are highly controlled environments, embryo culture conditions can still influence development. Temperature fluctuations, culture media quality, and oxygen levels can all impact embryo growth.
Tests Doctors Recommend After Poor Embryo Quality
When IVF cycles repeatedly produce poor-quality embryos or embryos that stop developing early, doctors often recommend additional investigations to identify the underlying cause. These tests help fertility specialists determine whether the issue is related to egg quality, sperm health, genetics, or other medical factors.
Ovarian Reserve Testing
Tests such as AMH (Anti-Müllerian Hormone) and antral follicle count help evaluate ovarian reserve. These tests provide insight into the number of eggs remaining in the ovaries and can guide IVF stimulation strategies.
Sperm DNA Fragmentation Test
Standard semen analysis evaluates sperm count and motility, but it does not measure DNA damage inside sperm cells. A sperm DNA fragmentation test can detect hidden damage that may affect embryo development.
Genetic Testing of Embryos (PGT-A)
Preimplantation Genetic Testing for Aneuploidy (PGT-A) analyzes embryos for chromosomal abnormalities before transfer. This test helps identify embryos with normal chromosome numbers, increasing the chances of implantation.
Hormonal and Metabolic Testing
Hormonal imbalances such as thyroid disorders, insulin resistance, or polycystic ovarian syndrome (PCOS) can indirectly affect egg quality and embryo development.
Advanced Genetic Screening
In rare cases, doctors may recommend genetic screening of both partners to identify inherited genetic conditions that may affect embryo viability.
How Doctors Try to Improve Embryo Quality in Future IVF Cycles
Experiencing poor embryo quality in one IVF cycle does not mean future cycles will fail. Fertility specialists often adjust treatment strategies to improve embryo development in subsequent attempts.
Personalized Ovarian Stimulation
Adjusting stimulation medications and protocols can improve the number and maturity of eggs retrieved during IVF.
Lifestyle Improvements
Factors such as smoking, alcohol consumption, obesity, and chronic stress may negatively affect egg and sperm quality. Lifestyle improvements can sometimes enhance reproductive health before the next IVF cycle.
Antioxidant and Nutritional Support
Some fertility specialists recommend antioxidants or nutritional supplements that support cellular health and reduce oxidative stress.
Improving Sperm Selection
Advanced sperm selection techniques such as PICSI or IMSI may help embryologists select healthier sperm for fertilization.
Laboratory Technology Improvements
Time-lapse embryo monitoring systems allow embryologists to observe embryo development continuously and select embryos with the most stable growth patterns.
Embryo Fragmentation Explained
One of the most common terms patients see in IVF laboratory reports is embryo fragmentation. Many couples are confused when they hear that their embryos have fragmentation, because the term is rarely explained in detail. Embryo fragmentation refers to small pieces of cellular material that appear between embryo cells during development. These fragments are not complete cells and do not contribute to normal embryo growth.
During early embryo development, cells should divide evenly and remain connected. When fragmentation occurs, parts of the cellular structure break off and accumulate around the embryo. A small amount of fragmentation is common and does not necessarily affect implantation. However, high levels of fragmentation may reduce the embryo’s ability to develop normally.
Fragmentation Grading
Embryologists often estimate fragmentation as a percentage of the embryo’s volume.
- 0–10% fragmentation: Excellent embryo quality
- 10–25% fragmentation: Mild fragmentation
- 25–50% fragmentation: Moderate fragmentation
- More than 50% fragmentation: Poor embryo quality
Embryos with high fragmentation levels may struggle to continue development or may stop growing before reaching the blastocyst stage. However, it is important to understand that fragmentation alone does not always determine whether an embryo will lead to pregnancy.
Why Fragmentation Happens
Several biological factors can contribute to embryo fragmentation:
- Chromosomal abnormalities in the embryo
- Poor egg quality
- Sperm DNA damage
- Errors during cell division
- Oxidative stress affecting reproductive cells
Understanding fragmentation is important because it helps doctors identify whether embryo development problems are related to egg quality, sperm health, or underlying genetic issues.
How IVF Laboratories Grade Blastocyst Embryos
When embryos reach the blastocyst stage on Day-5 or Day-6, embryologists evaluate them using a grading system that measures both structure and developmental potential. This grading system focuses on three key components of the blastocyst.
1. Blastocyst Expansion
Expansion refers to how much the embryo has grown and expanded its internal cavity. Blastocysts are typically scored from 1 to 6 depending on their level of expansion. Fully expanded blastocysts generally have higher implantation potential.
2. Inner Cell Mass (ICM)
The inner cell mass is the group of cells that will eventually develop into the baby. Embryologists evaluate whether these cells are tightly packed and healthy.
3. Trophectoderm (TE)
The trophectoderm forms the placenta and supports embryo implantation. Strong trophectoderm development improves the embryo’s ability to attach to the uterine lining.
Common Blastocyst Grades
- AA: Excellent embryo quality
- AB: Very good embryo
- BB: Good embryo with moderate potential
- BC or CC: Lower implantation potential
Even embryos with lower grades can still result in successful pregnancies. The grading system is only a tool used by doctors to estimate implantation potential.
When Embryo Quality Problems Are Not Fully Explained
Many couples who experience IVF failure feel confused about what went wrong. In some cases, the details of embryo quality are not fully explained during treatment. Patients may simply be told that the cycle “did not work” without receiving a clear explanation of embryo development, embryo grading, or possible biological causes.
Understanding embryo quality is important because it helps couples make informed decisions about future IVF cycles.
Questions Patients Should Ask Their IVF Clinic
- How many eggs were retrieved and how many fertilized?
- How many embryos developed to Day-3?
- How many embryos reached the blastocyst stage?
- What grades were assigned to the embryos?
- Did any embryos stop developing during culture?
- Were there signs of fragmentation or abnormal development?
Why These Questions Matter
These details can provide valuable insight into what happened during an IVF cycle and whether the problem may be related to egg quality, sperm health, genetics, or laboratory conditions.
Why Detailed IVF Case Review Matters
For couples who have experienced IVF failure, reviewing the full treatment history can reveal patterns that were not obvious during the initial cycle. Careful analysis of embryo development, laboratory reports, and medical history may help identify underlying causes and guide the next treatment strategy.
Signs Your IVF Cycle May Have Had Embryo Quality Problems
When an IVF cycle does not lead to pregnancy, many couples are told that the cycle simply “did not work.” However, in many cases the underlying reason is related to embryo development or embryo quality. Understanding the signs of embryo quality problems can help couples ask the right questions and plan better strategies for future IVF cycles.
Below are some of the most common patterns doctors observe when embryo quality may be affecting IVF success.
Few Embryos Reach the Blastocyst Stage
In a typical IVF cycle, several fertilized eggs should continue developing into blastocysts by Day-5 or Day-6. When most embryos stop growing earlier, it may suggest underlying biological problems affecting embryo development. Possible causes may include chromosomal abnormalities, poor egg quality, sperm DNA damage, or metabolic issues affecting embryo growth.
Embryos Stop Growing Between Day-3 and Day-5
One of the most common patterns seen in IVF laboratories is embryos that develop normally for the first few days but suddenly stop dividing around Day-3 or Day-4. This stage of development is important because the embryo begins activating its own genetic program. If chromosomal abnormalities or genetic instability are present, embryo development may stop at this stage.
Repeated Implantation Failure
Some patients undergo multiple IVF cycles where good-quality embryos are transferred but implantation does not occur. This situation is often referred to as repeated implantation failure. While uterine factors may sometimes play a role, embryo genetics is one of the most common reasons implantation fails repeatedly.
High Levels of Embryo Fragmentation
Embryologists often note fragmentation in embryo development reports. Fragmentation refers to small pieces of cellular debris surrounding embryo cells. High fragmentation levels may indicate abnormal cell division or genetic instability within the embryo.
Low Fertilization Rates
When only a small percentage of retrieved eggs fertilize successfully, it may indicate problems with egg quality or sperm health. Low fertilization rates can lead to fewer embryos available for development and transfer.
Poor Embryo Grades Across Multiple IVF Cycles
If several IVF cycles produce mostly low-grade embryos, it may indicate a consistent biological issue affecting embryo quality. Possible contributing factors may include:
- Declining egg quality
- Sperm DNA damage
- Chromosomal abnormalities
- Metabolic or hormonal factors
- Genetic compatibility issues
Why Identifying the Cause Matters
Understanding whether embryo quality played a role in IVF failure is important because treatment strategies can often be adjusted in future cycles.
Doctors may recommend changes such as different ovarian stimulation protocols, additional laboratory techniques, genetic testing, or lifestyle adjustments before the next IVF attempt. A careful review of previous IVF reports, embryo development records, and laboratory findings can provide valuable insights into what may have gone wrong and how treatment can be optimized for the next cycle.
Frequently Asked Questions About Embryo Quality
Can poor quality embryos still lead to pregnancy?
Yes. Lower grade embryos can still implant and develop into healthy babies. Embryo grading estimates implantation potential but does not guarantee success or failure.
Why do embryos stop growing during IVF?
The most common reason is chromosomal abnormalities. Other factors include egg quality, sperm DNA damage, and metabolic problems within the embryo.
Does embryo quality improve in the next IVF cycle?
In many cases yes. Doctors can adjust stimulation protocols, improve sperm selection, or recommend genetic testing to improve outcomes.
